How Long Does Suboxone Block Opiates?
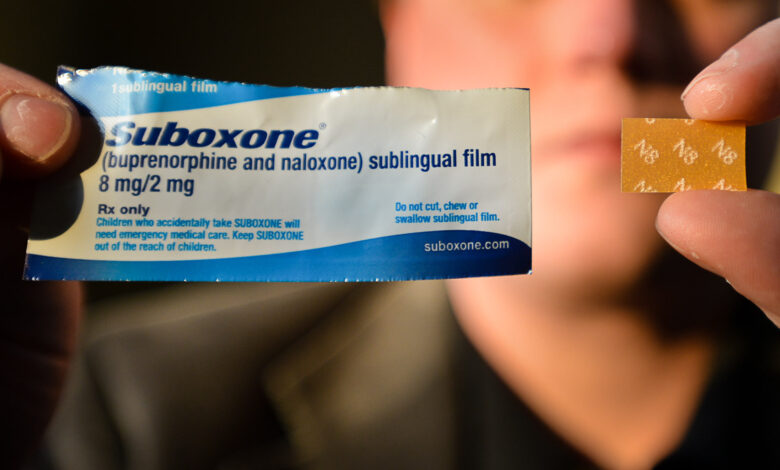
What is Suboxone and how does it work?
Suboxone, a combination medication containing buprenorphine and naloxone, is one of the main medications used to treat opioid addiction. Using ‘medications for opioid use disorder’ is known as MOUD. Use of MOUD has been shown to lower the risk of fatal overdoses by approximately 50%. It also reduces the risk of nonfatal overdoses which are traumatic and medically dangerous.
Suboxone works by tightly binding to the same receptors in the brain as other opiates, such as heroin, morphine, and oxycodone. By doing so, it blunts intoxication with these other drugs, it prevents cravings, and it allows many people to transition back from a life of addiction to a life of normalcy and safety.
A key goal of many advocates is to make access to Suboxone much more widely available, so that people who are addicted to opiates can readily access it. Good places to start are in the emergency department and in the primary care doctor’s office. More doctors need to become “waivered” to prescribe this medication, which requires some training and a special license.
The vast majority of physicians, addiction experts, and advocates agree: Suboxone saves lives. The U.S. Government has recently been lightening up on the requirements needed for doctors and nurses to “get waivered” in an urgent attempt to increase the availability of Suboxone prescribers, as the number of opioid deaths keeps rising.
How is Suboxone used?
Suboxone is available as a film to be placed either under the tongue or on the inside of the cheek, where it will dissolve in about 5 to 10 minutes.
Suboxone must be used under the supervision of a doctor who has experience in the management of opioid addiction. The medicine can only be obtained by ‘special’ prescription, which means it is used under stricter conditions than normal. This medicine can itself cause addiction so this measure is required to reduce misuse.
The precise way Suboxone is used depends on the patient’s status: type of addiction, state of withdrawal, and whether the patient is already using another substitution treatment such as methadone before starting Suboxone.
When starting treatment, Suboxone should be placed under the tongue. Once the patient is stabilized on a maintenance dose the film may also be placed inside the cheek. The recommended starting dose is 4 mg buprenorphine and 1 mg naloxone. The doctor may increase the dose depending on the patient’s response but the daily dose should not exceed 24 mg buprenorphine. Once the patient has been stabilized, the maintenance dose may be reduced gradually and eventually treatment may be stopped. The patient’s liver be checked before starting treatment with Suboxone and should also be monitored regularly during treatment. In patients who have mild to moderately reduced liver function lower starting doses are recommended. The effectiveness of Suboxone treatment depends on the patient also receiving other medical, social and psychological support.
How Long Does Suboxone Block Opiates?
Suboxone contains two active substances. Buprenorphine is a partial opioid agonist which means that it acts like an opioid drug. Naloxone is an opioid antagonist; this means that it counteracts the effects of opioid drugs.
Suboxone typically lasts up to 3 days. Most doctors ask their patients to take the drug once per day, typically at the same time each day. A person’s weight, metabolism, and history of drug abuse can lengthen or shorten the action of Suboxone. It’s best to work with a doctor on a customized dose, based on your medical history.
Expert practitioners have different theories on how long Suboxone treatment should last for, but there is no evidence to support the claim that Suboxone should be taken for a short period of time as opposed to being maintained on it for the long term, just as a person would manage their diabetes with insulin for the long term. Ultimately, this comes down to patient preference.
One of the main obstacles to getting lifesaving treatment for addiction is the stigma people face. Fortunately, our society’s perception is slowly starting to transform away from an outdated view of addiction as a moral failing, toward a more realistic, humane view of addiction as a complex disease that needs to be addressed with compassion, as well as modern medical care. Eliminating myths and misinformation about addiction, and supplanting them with up-to-date, evidence-based treatments, is a critical step in the evolution and improvement of addiction treatment.