Methotrexate: Uses, How it Works, Dosage, Side Effects, Reviews

Methotrexate (MTX), sold under the brand names Rheumatrex®, Trexall® and others is a strong medication used to treat certain types of cancer such as leukemia, non-Hodgkin’s lymphoma, breast cancer, head and neck cancer, stomach cancer, bladder cancer, bone cancer, and choriocarcinoma (a type of uterine cancer). It is also used to treat rheumatoid arthritis, psoriatic arthritis, and psoriasis (a chronic skin disorder that produces patchy scales) when other treatments have not provided a satisfactory result.
When used to treat cancer, methotrexate works by blocking an enzyme process in cancer cells so they cannot grow. Used for this purpose, methotrexate is known as an anti-metabolite.
For rheumatoid arthritis, it works by reducing inflammation and by suppressing the immune system. For psoriasis, methotrexate works by attacking the rapidly dividing cells that are involved in causing psoriasis. Under these circumstances, methotrexate is known as a disease-modifying antirheumatic drug (DMARD).
How should methotrexate be used?
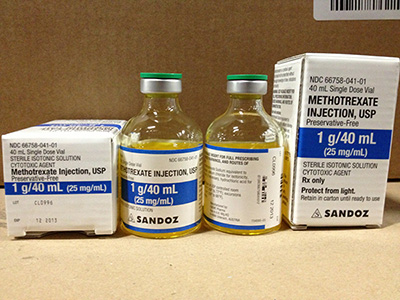
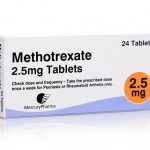
Methotrexate comes as a tablet to take by mouth and also as an injection. Your doctor will tell you how often you should take methotrexate. The schedule depends on the condition you have and on how your body responds to the medication.
Your doctor may tell you to take methotrexate on a rotating schedule that alternates several days when you take methotrexate with several days or weeks when you do not take the medication. Follow these directions carefully and ask your doctor or pharmacist if you do not know when to take your medication.
Methotrexate injection comes as a powder to be mixed with liquid to be injected intramuscularly (into a muscle), intravenously (into a vein), subcutaneously (just under the skin), or intrathecally (into the fluid-filled space of the spinal canal). The length of treatment depends on the types of drugs you are taking, how well your body responds to them, and the type of cancer or condition you have.
If you are taking methotrexate to treat psoriasis or rheumatoid arthritis, your doctor may tell you to take the medication once a week. Pay close attention to your doctor’s directions. Some people who mistakenly took methotrexate once daily instead of once weekly experienced very severe side effects or died.
Follow the directions on your prescription label carefully, and ask your doctor or pharmacist to explain any part you do not understand. Take methotrexate exactly as directed. Do not take more or less of it or take it more often than prescribed by your doctor.
Ask your pharmacist or doctor for a copy of the manufacturer’s information for the patient

What Are the Side Effects of Methotrexate?
Side effects of Methotrexate include:
• inflammation of the mouth and lips,
• nausea,
• vomiting,
• upset stomach,
• abdominal pain,
• dizziness,
• tired feeling,
• headache,
• bleeding gums,
• blurred vision, and
• leukopenia (low number of white cells in blood).
Tell your doctor if you have serious side effects of Methotrexate including:
• dry cough,
• shortness of breath,
• diarrhea,
• white patches or sores inside your mouth or on your lips,
• blood in your urine or stools,
• urinating less than usual or not at all,
• fever,
• chills,
• body aches,
• flu symptoms,
• sore throat and headache with a severe blistering/peeling/red skin rash,
• pale skin,
• easy bruising or bleeding,
• weakness,
• stomach pain,
• loss of appetite,
• dark urine,
• clay-colored stools, or
• jaundice (yellowing of the skin or eyes).
Severe side effects occur more frequently in patients taking the high doses of methotrexate.
What other drugs could interact with methotrexate?
There may be an interaction between methotrexate and any of the following:
• acitretin
• alcohol
• alitretinoin
• aminoglycosides (e.g., gentamicin, tobramycin)
• amphotericin B
• azathioprine
• “azole” antifungals (e.g., itraconazole, ketoconazole, voriconazole)
• baricitinib
• carbamazepine
• celecoxib
• chloral hydrate
• cholestyramine
• ciprofloxacin
• clozapine
• colesevelam
• colestipol
• cyclosporine
• daclatasvir
• deferiprone
• denosumab
• dexamethasone
• dronedarone
• echinacea
• eltrombopag
• fingolimod
• folic acid
• foscarnet
• furosemide
• gemfibrozil
• HIV protease inhibitors (e.g., atazanavir, indinavir, ritonavir, saquinavir)
• leflunomide
• live vaccines (e.g., BCG, yellow fever, measles, mumps, rubella)
• macrolide antibiotics (e.g., clarithromycin, erythromycin)
• mefloquine
• nonsteroidal anti-inflammatory medications (NSAIDs; e.g., diclofenac, ibuprofen, ketoprofen, naproxen)
• ocrelizumab
• other cancer medications (e.g., cytarabine, doxorubicin, vinblastine)
• penicillins (e.g., amoxicillin, ampicillin, penicillin, cloxacillin)
• phenobarbital
• phenytoin
• pimecrolimus
• protein kinase inhibitors (e.g., lapatinib, nilotinib, sunitinib)
• proton pump inhibitors (e.g., lansoprazole, omeprazole)
• quinidine
• quinine
• retinoids (e.g., tretinoin, retinol)
• rifampin
• roflumilast
• salicylates (e.g., ASA, salsalate)
• sulfonamide antibiotics (e.g., sulfasalazine, sulfamethoxazole, sulfadiazine)
• sulfasalazine
• tacrolimus
• tegafur
• tenofovir
• teriflunomide
• tetracyclines (e.g., doxycycline, minocycline, tetracycline)
• theophyllines (e.g., aminophylline, oxtriphylline, theophylline)
• tolvaptan
• trazodone
• trimethoprim
• vancomycin
• velpatasvir
• verapamil
• warfarin
If you are taking any of these medications, speak with your doctor or pharmacist. Depending on your specific circumstances, your doctor may want you to:
• stop taking one of the medications,
• change one of the medications to another,
• change how you are taking one or both of the medications, or
• leave everything as is
An interaction between two medications does not always mean that you must stop taking one of them. Speak to your doctor about how any drug interactions are being managed or should be managed.



One Comment