Why is Levemir Given at Night?

Levemir is a man-made form of insulin, a hormone that is produced in the body. It’s used to lower blood sugar levels in adults and children ages 2 years old and older with type 1 diabetes as well as adults with type 2 diabetes Levemir has not been studied in children younger than 2 years of age with type 1 diabetes. It also hasn’t been studied in any children younger than 18 years of age with type 2 diabetes.
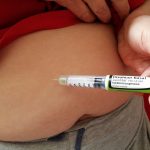
Levemir contains the drug insulin detemir, which is a long-acting insulin. Levemir is given as a subcutaneous injection (under the skin). You’ll give yourself injections either once or twice a day based on your doctor’s or pharmacist’s direction. Levemir comes as a solution (liquid mixture). The solution is available in two forms: a vial and a prefilled pen.
The vial contains 10 milliliters (mL) of drug solution, with 100 units of insulin detemir per mL. It’s used with a needle for injection. Needles are sold separately and may require a prescription in certain states. The pen is called the FlexTouch pen. Each pen contains 3 mL of drug solution, with 100 units of insulin detemir per mL.
How does Levemir work?
Insulin works by lowering levels of glucose (sugar) in the blood. Levemir is a long-acting insulin that starts to work several hours after injection and keeps working evenly for up to 24 hours. In clinical studies, adults with type 1 diabetes who took Levemir had their hemoglobin A1c (HbA1c) lowered by an average of 0.1% to 0.8%. In comparison, adults who took either insulin NPH (an intermediate-acting insulin) or insulin glargine (Lantus), a long-acting insulin, had their HbA1c lowered by an average of 0% to 0.7%.
In clinical studies, adults with type 2 diabetes taking Levemir had their HbA1c lowered by an average of 0.6% to 2%. In comparison, people who took insulin NPH saw a reduction in HbA1c of an average of 0.6% to 2.1%. Levemir also lowered fasting blood sugar by an average of 69 mg/dL over 24 weeks. In comparison, people taking insulin NPH had their fasting blood sugar lowered by an average of 74 mg/dL.
How Levemir is used
For proper storage, opened vials should be kept in the fridge, while opened pens should be kept at room temperature.
Inject at the same time each day, but rotate injection sites to prevent skin irritation or deformity.
For proper use, inject Levemir (insulin detemir) under your skin (subcutaneously) in your upper arm, abdomen (stomach area), or thigh (upper leg).
Never inject it into a vein or muscle. This can cause severely low blood sugar levels and infections.
Do not dilute or mix with other types of insulin; it will not work as intended and you may lose blood sugar control, which could be serious. However, your doctor may prescribe other short-acting insulins to use at different times of the day depending on your blood sugar control.
Keep a consistent meal and exercise schedule to prevent any fluctuations in your blood sugar.
Do not re-use needles. Always use a new needle for each injection. Reusing needles increases your chance of having blocked needles, which can cause you to get the wrong dose of Levemir (insulin detemir). Using a new needle for each injection also lowers your risk of getting an infection.
When changing to Levemir (insulin detemir) from other basal insulins you may experience higher average fasting blood sugar levels in the first weeks of therapy. Monitor sugar levels daily to ensure that they are within a healthy range.
The following are some common symptoms of low blood sugar: feeling shaky, being nervous or anxious, fast heartbeat, sweating or body chills, confusion, feeling sleepy, weakness or low energy and excessive hunger.
If your blood sugar ever gets too low (between 50 and 70 mg/dL), then it is important that you eat 15 grams of fast-acting sugar to bring your blood sugar back above 70 mg/dL. Some examples of fast-acting sugar include: 4 glucose (sugar) tablets, 3-4 pieces of hard candy, one-half cup of fruit juice, or one-half can of regular soda. After eating 15 grams of fast-acting sugar, wait 15 minutes and recheck your blood sugar. If it is still below 70 mg/dL then eat another 15 grams of carbohydrates and recheck again in 15 minutes. Once your blood sugar is above 70 mg/dL, then eat a meal to keep your blood sugars in a normal range. If your blood sugar is not rising when you eat or your blood sugar drops even lower after eating, call 911.
Why Take Levemir At Night?
Levemir is best given with the evening meal or at bedtime. When taken twice daily, the evening dose should be taken with the evening meal, at bedtime, or 12 hours following the morning dose, this is because basal insulin which keep blood sugar levels within the normal range should produce at most a 30 milligrams per deciliter (mg/dL) change when blood sugar levels are stable and in your target range during sleep times. That’s why your healthcare provider will most likely advise you to inject Levemir at night, preferably before bedtime.
In addition, weight gain and night-time hypoglycemia (low blood sugar levels) appear to be less with Levemir.
Top 10 List of Safety Tips for Levemir
When taking your medicine:
1. Know your insulin. Levemir is a long-acting insulin that should be injected below the skin once or twice daily. (When taken in smaller doses, Levemir may be considered an intermediate-acting insulin). When Levemir is taken once daily, inject the insulin with the evening meal or at bedtime. When taken twice daily, the evening dose should be taken with the evening meal, at bedtime, or 12 hours following the morning dose.
2. Prepare your insulin. A rapid- or short-acting insulin is often prescribed with Levemir. However, Levemir should never be mixed in the same syringe with other insulins before injection. Do not vigorously shake insulin before use.
3. Don’t reuse or recycle. Discard used syringes/needles, pens, and lancets in a sealable hard plastic or metal container (e.g., empty detergent bottle, sharps container from your pharmacy). When the container is full, seal the lid before placing it in the trash. Don’t reuse or recycle syringes, needles, or lancets.
4. Don’t share. Even if you change the needle, sharing an insulin pen or syringe may spread diseases carried in the blood, including hepatitis and HIV.
To avoid serious side effects
5. Avoid mix-ups. If you use more than one type of insulin, make sure each vial, pen, or cartridge looks different. If insulins look similar, put a rubber band around one type to help avoid mix-ups.
6. Check your medicine. There are dozens of different insulins on the market, many in similar looking vials, cartons, or pens. When you pick up your insulin at the pharmacy, be sure it’s the right type of insulin.
7. Treat low blood sugar (hypoglycemia). Carry a quick source of sugar, such as glucose tablets, candy, or juice, to treat low blood sugar. Signs of low blood sugar are listed below.
8. Test your blood sugar level. Ask your doctor how often you should test your blood sugar level. Keep a log of your blood sugar levels and how much insulin you take each day. Bring the log with you each time you visit your doctor.
9. Get a periodic lab test. You should have a hemoglobin A1c test at least twice a year to determine how well your diabetes is being controlled. The test shows an average of your blood sugar control over a 6- to 12-week period. Your goal is a hemoglobin A1c of 7% or less.
When you should call your doctor
10. Call for illness or changes in habits. Your insulin needs may change because of illness, stress, changes in eating habits or physical activity, and other medicines you take. Call your doctor if you experience these conditions. Never change your insulin dose unless advised by your doctor.
You may find useful information on: FDA Approves Semglee The First Interchangeable Biosimilar Insulin