Diabetes Test Less Reliable In Black Patients
The discovery of a genetic variation common among people of African ancestry, known as G6PD deficiency (G6PDdef), has significant implications for the reliability of a widely used blood test for diagnosing diabetes. This breakthrough, reported in Nature Medicine, highlights a critical factor contributing to the higher risks of delayed diabetes diagnoses and complications in Black patients. The variant’s association with a shorter red blood cell lifespan impacts hemoglobin A1c (HbA1c) levels, a key marker used to diagnose diabetes, thus making the standard test less reliable for this population.
G6PD deficiency leads to lower levels of hemoglobin A1c in individuals, which can result in HbA1c levels falling below the diagnostic threshold for diabetes. Consequently, these individuals may not receive timely or appropriate treatment, despite having high blood sugar levels that are sufficiently elevated to cause diabetes-related complications. This discrepancy can delay the introduction of treatments ranging from oral medications like metformin to insulin injections, increasing the risk of damage to critical organs such as the eyes, nerves, and kidneys.
The research team, by analyzing genetic data from over 200,000 individuals with diabetes, observed that those with G6PDdef had significantly higher blood glucose levels and lower HbA1c levels both in the year preceding a diabetes diagnosis and in the year prior to receiving their first insulin prescription. These individuals also faced higher risks of developing diabetic eye disease and nerve damage, even when receiving standard diabetes care. This suggests that the current reliance on HbA1c levels as a primary diagnostic tool may not be sufficient for individuals with this genetic variation.
In the United States, it is estimated that more than 250,000 men and 500,000 women of non-Hispanic African ancestry who have diabetes may have some degree of G6PD deficiency. This prevalence underscores the need for a reevaluation of diagnostic and treatment strategies for diabetes within this population. The researchers suggest that comprehensive screening for G6PD deficiency, coupled with treatment protocols aimed more directly at managing blood glucose levels rather than HbA1c levels, could significantly reduce the incidence of diabetes-related complications. They estimate that such an approach could potentially prevent nearly 12% of diabetic retinopathy cases and 9% of diabetic neuropathy cases in non-Hispanic African Americans in the U.S.
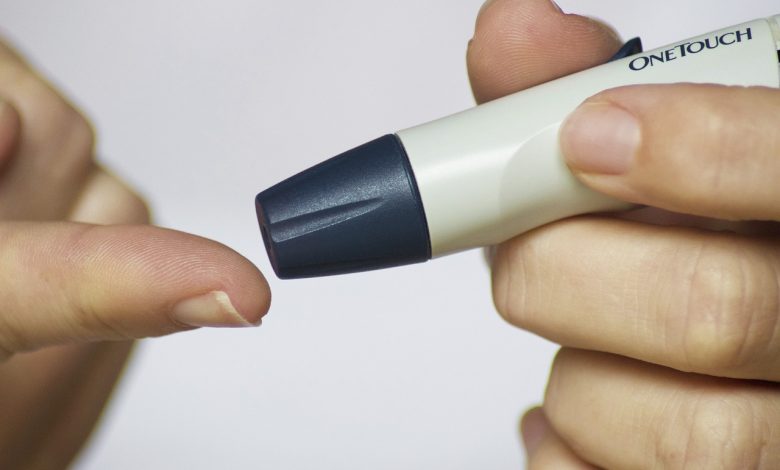
The current standard for diagnosing diabetes involves measuring HbA1c levels, which reflect average blood sugar levels over the past two to three months. However, in individuals with G6PD deficiency, the shorter lifespan of red blood cells results in lower HbA1c levels, which may not accurately represent their true blood glucose levels. This can lead to underdiagnosis or delayed diagnosis, preventing timely intervention that could mitigate the risk of severe complications.
The findings from this study advocate for the inclusion of genetic screening as part of routine diabetes care, particularly for populations at higher risk of G6PD deficiency. By identifying individuals with this genetic variation, healthcare providers can tailor their diagnostic and treatment approaches, ensuring that blood glucose levels are effectively managed. This personalized approach to diabetes care could help bridge the gap in health disparities observed between individuals of European and African ancestries.
Moreover, the research emphasizes the importance of recognizing and addressing genetic diversity in medical diagnostics and treatment. The reliance on HbA1c as a universal marker for diabetes may not be suitable for all populations, and understanding genetic differences can lead to more accurate and equitable healthcare outcomes. As genetic testing becomes more accessible and affordable, it has the potential to transform diabetes care, making it more inclusive and effective.
In conclusion, the discovery of the G6PD deficiency variant’s impact on HbA1c levels in individuals of African ancestry represents a significant advancement in our understanding of diabetes diagnostics. By incorporating genetic screening into routine care and focusing treatment strategies on blood glucose levels, healthcare providers can improve the accuracy of diabetes diagnoses and reduce the risk of complications in this population. This approach not only enhances individual patient outcomes but also contributes to reducing health disparities and promoting equity in healthcare.