Is 20 Units Of Insulin A Lot?
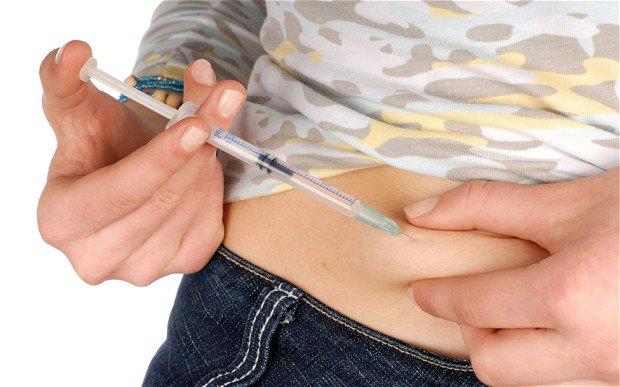
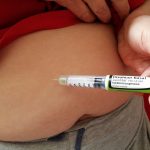
Insulin is a naturally occurring hormone made by the pancreas that helps the body use or store the glucose (sugar) it gets from food. For people with diabetes, either the pancreas does not make enough insulin to meet the body’s requirements, or the body cannot properly use the insulin that is made. As a result, glucose cannot be used or stored properly and accumulates in the bloodstream. Insulin injected under the skin helps to lower blood glucose levels.
There are many different types of insulin and they are absorbed at different rates and work for varying periods of time. Regular insulin is a short-acting insulin. It takes 30 to 60 minutes to begin working after injection, and has its maximum effect between 2 and 4 hours after injection. It stops working after 6 to 8 hours. This medication may be available under multiple brand names and/or in several different forms.
According to the American Academy of Family Physicians, the several different types of insulin that people can use separately or in combination.
These include:
- Rapid-acting insulins that start to work within 15 minutes and can last around 3–5 hours.
- Short-acting insulins that take 30–60 minutes to start working and have a duration of 5–8 hours.
- Intermediate-acting insulins that take 1–3 hours to start working but last 12–16 hours.
- Long-acting insulins that start to work in about 1 hour and can last 20–26 hours.
- Premixed insulins that combine a rapid- or short-acting insulin with a longer-lasting one.
A doctor will prescribe one of these insulins or a mixture alongside a carefully controlled schedule. Following this closely will reduce the risk of side effects and complications.
How should I use this medication?
Your required dose of regular insulin depends on how much natural insulin your pancreas is producing and how well your body is able to use it. Your doctor or diabetes educator will determine the appropriate dose for you according to various lifestyle factors and the blood glucose values obtained while monitoring your blood glucose.
Your dose of regular insulin should be injected subcutaneously (under the skin) exactly as instructed by your doctor or diabetes educator. Do not inject regular insulin into the vein and do not use regular insulin in insulin infusion pumps. The dose of insulin is measured in international units (IU). Each mL of insulin contains 100 IU. Regular insulin is injected about 30 minutes before certain meals. Longer-acting insulins are often used along with regular insulin to cover the time between doses of regular insulin. There are many variations of insulin dosing.
Is 20 Units Of Insulin A Lot?
According to Russell D. White, MD a Professor of Medicine and Director, Sports Medicine Fellowship Program University of Missouri–Kansas City School of Medicine, When it comes to using insulin to treat hyperglycemia, “the sky’s the limit.” Extremely high doses are occasionally required; that is the reason U-500 insulin is available. A colleague once reported using 35,000 units of insulin a day in a patient with a genetic receptor defect. In patients with glucotoxicity, hyperglycemia, and down-regulation of the beta cells, very high doses of insulin are needed to reverse the clinical situation; after this has been accomplished, the insulin dose can be gradually lowered to a maintenance level. Ironically, hyperglycemia may either stimulate the beta cells to correct the clinical problem or have a toxic effect on the beta cells (i.e., induce apoptosis) and thus worsen the situation.
In patients with type 2 diabetes, marked obesity, and insulin resistance, total daily insulin doses of 200 to 300 units are often required. In this setting, management for most patients includes a total of 1.0 to 2.0 units of insulin per kilogram per day; thus, in very obese patients, a larger total dose is required. In these patients-provided they have no contraindication-metformin therapy is continued by most clinicians to treat insulin resistance, improve glucose control, and minimize further weight gain.
In general, many things can affect the dose of medication that a person needs, such as body weight, other medical conditions, and other medications. If your doctor has recommended a dose different from the ones given here, do not change the way that you are using the medication without consulting your doctor.
It is very important that you use this medication exactly as prescribed by your doctor. The timing of insulin with respect to your meals is crucial to keeping blood glucose under control and preventing unwanted side effects.
Keep unopened bottles of insulin in the refrigerator until needed. They may be used until the expiry date on the label. Never allow insulin to freeze. Insulin that is currently in use may be kept at room temperature for no more than 28 days and then discarded. Do not expose insulin to extremely hot temperatures or to sunlight. Keep insulin out of the reach of children.
What is the average dose of insulin for type 2 diabetes?
According to WebMD, when it comes to long-acting insulin, each has its own dosage. Depending on the type, you might start with 10 units a day. Or your doctor may base the first dose on your weight, based on about 0.2 units for every 2.2 pounds. On how many units of insulin is normal, that depends on the amount of insulin a patient is producing and the condition being treated. So…. is 32, 40 or 45 units of insulin a lot? No, the maximum insulin dose per day is dependent on what your doctors consider appropriate for your condition.
What are the side effects of Human insulin?
Human insulin causes changes in your blood sugar. You should know the symptoms of low and high blood sugar and what to do if you have these symptoms.
This medication may cause side effects. Tell your doctor if any of these symptoms are severe or do not go away:
• redness, swelling, and itching at the injection site
• changes in the feel of your skin, skin thickening (fat build-up), or a little depression in the skin (fat breakdown)
• weight gain
• constipation
Some side effects can be serious. If you experience any of the following symptoms, call your doctor immediately:
• rash and/or itching over the whole body
• shortness of breath
• wheezing
• dizziness
• blurred vision
• fast heartbeat
• sweating
• difficulty breathing or swallowing
• weakness
• muscle cramps
• abnormal heartbeat
• large weight gain in a short period of time
• swelling of the arms, hands, feet, ankles, or lower legs
If you experience a serious side effect, you or your doctor may send a report to the Food and Drug Administration’s (FDA) MedWatch Adverse Event Reporting program online (http://www.fda.gov/Safety/MedWatch) or by phone (1-800-332-1088).
You may find useful information on: Why is Levemir Given at Night?