Naloxone (Narcan, Evzio) Uses, Mechanism of Action, Dosage, Side Effects
What Is Naloxone And What Does It Treat?
Naloxone is a medication in a class of drugs called opiate antagonists designed to rapidly reverse opioid overdose. Naloxone reverses/block the effects of other opioids such as heroin or certain pain medications (e.g., oxycodone, morphine, hydrocodone). After administering naloxone, you should still immediately seek emergency medical care.
Naloxone has no effect on people who have not taken opioids.
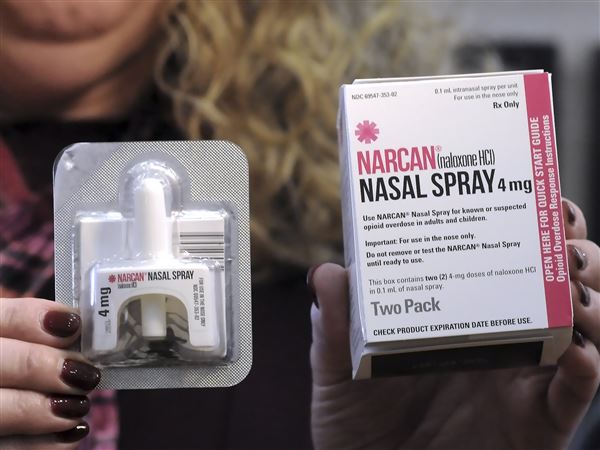
Narcan® is a nasal spray form of naloxone. A generic formulation is available. Naloxone is also available as an auto-injectable device with an electronic voice instruction system named Evzio®.
How Naloxone works
Naloxone works by reversing the effects of opioid analgesics by binding to the opioid receptors in the CNS and inhibiting the typical actions of opioid analgesics, including analgesia, euphoria, sedation, respiratory depression, miosis, bradycardia, and physical dependence.
How Long Does It Take For Naloxone To Work?
Depending on the opioids overdosed, naloxone should show a response in 2 to 3 minutes. Otherwise, the medication can be readministered until medical services arrive or the patient responds positively.
Who Should Have Naloxone On Hand?
Anyone can carry naloxone on hand in case of emergencies.
Some populations that may particularly benefit include:
• Anyone who is taking opioids or is at risk of an overdose
• Family, friends, or acquaintances of someone who may be at risk of an opioid overdose
• Healthcare professionals
• First responders, including police, firefighters, and EMTs
All 50 states and the District of Columbia permit pharmacy-based naloxone dispensing with a prescription from a physician. Most states allow for behind-the-counter (without a prescription) naloxone purchases. Please check with your local pharmacy for pertinent legal information.
What Is The Most Important Information I Should Know About Naloxone?
Naloxone is a drug used in an emergency to reverse an opioid overdose. Naloxone is not a replacement for emergency medical care for an overdose. Even if the patient wakes up or improves, you should still seek emergency medical assistance.
If the patient is opioid-dependent, the use of naloxone may cause opioid withdrawal. Signs of opioid withdrawal include body aches, diarrhea, fast heart rate, high blood pressure, fever, and irritability.
Can a pregnant woman use Naloxone?
There is limited data on naloxone use in pregnant women to inform about drug-associated risk. It is important to discuss the risks and benefits of continued treatment with your doctor and caregivers.
Naloxone crosses the placenta and may precipitate withdrawal in the fetus, in addition to the opioid-dependent mother. The fetus should be evaluated for signs of distress after naloxone is used.
Naloxone did not appear to cause birth defects during animal studies.
There is no information regarding the presence of naloxone in human milk or its effects on breastfed infants or on milk production. Naloxone does not affect prolactin or oxytocin hormone levels.
What Should I Discuss With My Health Care Provider Before Taking Naloxone?
• If you have allergies to any medications
• Any other psychiatric or medical problems you have, including a history of heart problems
• All other medications you are currently taking (including over the counter products, herbal and nutritional supplements)
• Other non-medication treatments you are receiving, such as talk therapy or counseling. Your provider can explain how these different treatments work with the medication.
• If you are pregnant, plan to become pregnant, or are breastfeeding
• If you use illegal drugs or narcotics
How Do I Identify An Opioid Overdose?
Signs and symptoms of an opioid overdose may include:
• Loss of consciousness, unusual sleepiness, and/or inability to respond to loud voices or touch
• Breathing problems such as slow, shallow, or cessation of breathing
• The black circle in the center of the eye (pupil) becomes very small (pinpoint pupils)
Certain people are at an increased risk for an opioid overdose:
• People with opioid use disorder
• People who may have a reduced opioid tolerance (following detoxification, release from incarceration, cessation of treatment)
• People who use prescription opioids, in particular, those taking higher doses
• People who use opioids in combination with other sedating substances (such as alcohol or benzodiazepines)
• Household members of people in possession of opioids (including prescription opioids)
How Should I Administer Naloxone?
Depending on the state you live in, friends, family members, and others in the community may give naloxone to someone who has overdosed.
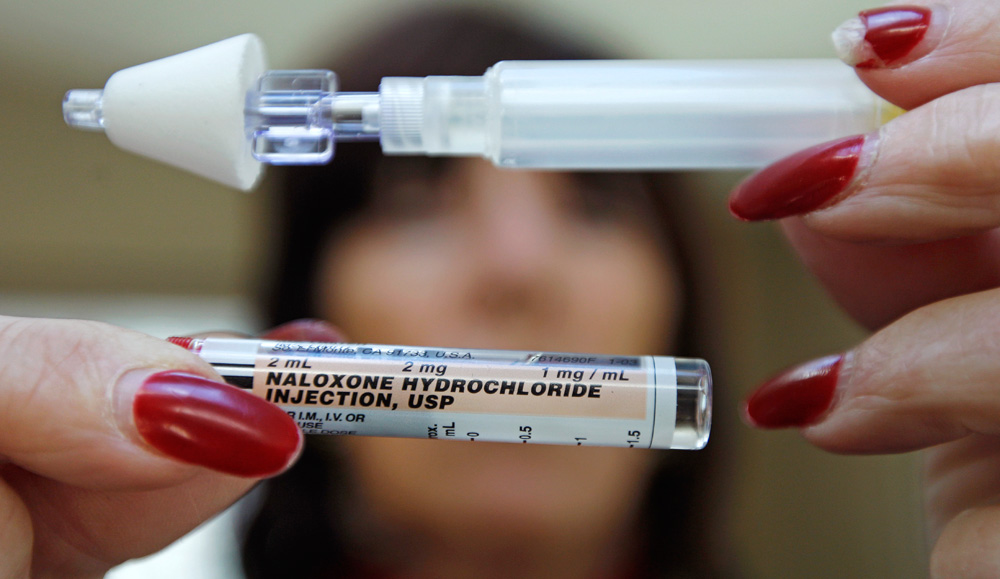
Evzio® is a prefilled auto-injection device. Each device contains a single dose of naloxone and cannot be reused. Once activated, the device provides verbal instruction to the user. The device should be injected into the muscle or skin of the outer thigh and if necessary, Evzio® may be injected through clothing (i.e., pants or jeans). If symptoms return, additional doses may be administered every 2 to 3 minutes until emergency services arrive or the patient responds positively.
Narcan® is a prefilled nasal spray. It is also available in generic formulations. Each device contains a single dose of naloxone that cannot be reused. When administering the spray, the patient should be placed flat on their back, with their head tilted back, supporting the neck. The first dose is given as one spray into one nostril. If there is no recovery in 2-3 minutes, the dose is repeated in the other nostril. The spray may be repeated every 2 to 3 minutes in alternating nostrils until emergency services arrive or the patient responds positively.
Naloxone does not take the place of emergency medical care. Emergency medical services should be contacted and CPR may be performed on the patient.
What Should I Avoid While Taking Naloxone?
Since naloxone is an opioid blocker designed to rapidly reverse opioid overdose, it can cause withdrawal symptoms if used in patients who are dependent on opioids. It should be used in an emergency situation if a patient is unresponsive and opioid overdose is suspected. Naloxone has no effect on people who have not taken opioids.
What Are The Possible Side Effects Of Naloxone?
In patients who have been using opioids regularly, opioid withdrawal symptoms can occur after receiving naloxone. Opioid withdrawal symptoms include: body aches, fever, sweating, running nose, sneezing, goosebumps, yawning, weakness, shivering or trembling, nervousness, restlessness or irritability, diarrhea, nausea, vomiting, stomach cramping, increased blood pressure, and increased heart rate.
Common side effects of Evzio® include dizziness and injection site redness.
What Other Medications May Interact With Naloxone?
Naloxone may interact with certain cough/cold medications and anti-diarrheal medications. Your pharmacist or doctor will help you to determine if other medications you take can interfere with the effects of naloxone.
How Should Naloxone Be Stored?
Naloxone nasal spray and the auto-injectable device should be stored at room temperature. Replace the auto-injectable device if the solution is discolored or contains a precipitate. Do not freeze products.
How much does naloxone cost?
The cost varies depending on where you get the naloxone, how you get it, and what type you get. Patients with insurance should check with their insurance company to see if this medicine is covered. Patients without insurance can check the retail costs at their local pharmacies. Some drug companies have cost assistance programs for patients unable to pay for it.
Where can I get naloxone?
Many pharmacies carry naloxone. In some states, you can get naloxone from a pharmacist even if your doctor did not write you a prescription for it. It is also possible to get naloxone from community-based distribution programs, local public health groups, or local health departments, free of charge.