Medications That Can Cause Deep Vein Thrombosis (DVT)
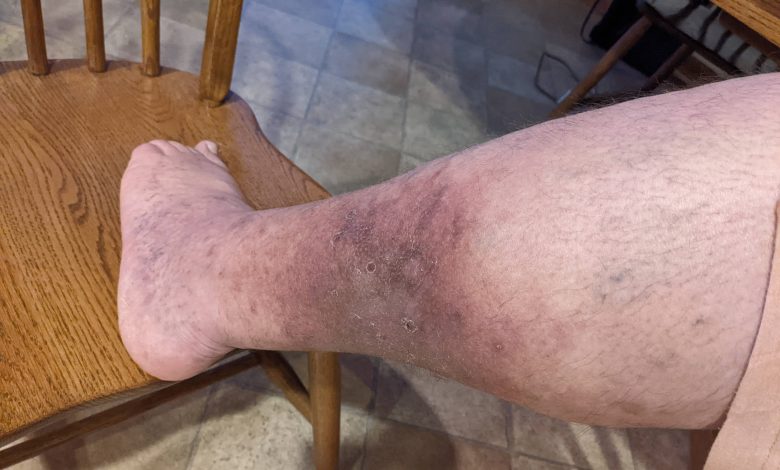
Deep vein thrombosis (DVT) is a medical condition characterized by the formation of blood clots within deep veins, typically in the legs. This condition poses a serious health risk as these clots have the potential to break loose and travel through the bloodstream, reaching the lungs, where they can cause a life-threatening condition known as pulmonary embolism. DVT often occurs when there is a disruption in normal blood flow, such as during prolonged immobility, surgery, or trauma. Individuals with certain medical conditions or a family history of blood clotting disorders may also be at an increased risk of developing DVT.
The symptoms of DVT can vary, and some individuals may experience no symptoms at all. Common signs include swelling, pain, and tenderness in the affected leg, typically in the calf. The affected area may also appear red or warm to the touch. It’s essential to note that these symptoms may not be exclusive to DVT and can be indicative of other conditions, making it crucial for individuals experiencing these symptoms to seek medical attention promptly. In some cases, DVT can be asymptomatic, highlighting the importance of preventive measures and awareness, particularly for those at higher risk.
While there are various risk factors associated with DVT, including genetics, surgery, and prolonged immobility, the role of certain medications in contributing to the development of DVT cannot be overlooked. Annually, an estimated 1 to 3 in every 1,000 adults in the United States develop DVT resulting in up to 300,000 deaths each year. This staggering statistic emphasizes the critical need for comprehensive awareness and proactive management of factors that may contribute to blood clot formation. DVT ranks as the third most common vascular disease, trailing only behind heart attacks and strokes. Given its substantial public health burden, it becomes imperative for healthcare professionals and patients alike to delve into the intricate relationship between medications and DVT, recognizing the nuances that can significantly impact patient outcomes. This article explores the connection between medications and DVT, shedding light on the drugs that may pose a risk and the mechanisms by which they can increase the likelihood of blood clot formation.
Anticoagulants and Antiplatelet Medications
Ironically, some medications that are commonly prescribed to prevent blood clots may also have the potential to cause DVT in certain circumstances. Anticoagulants and antiplatelet drugs, which are often prescribed to individuals at risk of cardiovascular events, work by thinning the blood and inhibiting clot formation. While these medications play a crucial role in preventing conditions like stroke and heart attack, they may pose a risk of bleeding, especially if the dosage is not carefully monitored.
Warfarin, a widely used anticoagulant, has been associated with an increased risk of DVT when not properly managed. The delicate balance required to achieve therapeutic anticoagulation without causing bleeding complications makes warfarin management challenging. Patients on warfarin need regular monitoring of their International Normalized Ratio (INR) to ensure that their blood is neither too thin nor too thick.
Hormonal Medications
Hormonal medications, particularly oral contraceptives and hormone replacement therapy (HRT), have been linked to an elevated risk of DVT. Estrogen, a key component in these medications, is known to influence blood clotting factors. The use of hormonal contraceptives, especially in combination with other risk factors like smoking and obesity, can significantly increase the likelihood of developing DVT. It is important for healthcare providers to assess an individual’s overall risk profile before prescribing hormonal medications, and patients should be educated about the potential risks and benefits.
Certain medical conditions, such as cancer, may also require hormone therapy. Cancer patients often undergo treatments that can increase the risk of clot formation. It is crucial for healthcare professionals to carefully weigh the risks and benefits of hormonal therapies in such cases, implementing preventive measures when necessary.
Immune System Modulators
Some medications that modulate the immune system, such as certain chemotherapy drugs and monoclonal antibodies, have been associated with an increased risk of DVT. These drugs are often used in the treatment of autoimmune disorders and certain cancers. While they play a vital role in managing these conditions, they may disrupt the balance of the coagulation system, potentially leading to the formation of blood clots.
Chemotherapy drugs, in particular, can cause damage to blood vessels and trigger inflammatory responses, increasing the risk of clot formation. Patients undergoing immune-modulating therapies should be closely monitored for signs of DVT, and healthcare providers should consider preventive measures such as the use of anticoagulants when deemed appropriate.
Psychotropic Medications
Psychotropic medications, including certain antidepressants and antipsychotics, have also been implicated in the development of DVT. While the exact mechanisms are not fully understood, these medications may influence the coagulation cascade and increase the risk of clot formation. Additionally, individuals with mental health conditions may already have an increased risk of cardiovascular issues, further emphasizing the importance of a comprehensive risk assessment before prescribing psychotropic medications.
It is essential for healthcare providers to carefully evaluate the risk-benefit profile of psychotropic medications, taking into consideration both the mental health needs of the patient and their overall cardiovascular risk. Regular monitoring and communication between the patient and healthcare team are crucial to identify and address any emerging concerns promptly.
Conclusion
The relationship between medications and Deep Vein Thrombosis is complex and multifaceted. While some drugs are known to increase the risk of DVT, it’s crucial to recognize that the interaction between medications and individual patient factors plays a significant role in determining the overall risk. Healthcare providers must carefully assess each patient’s medical history, underlying conditions, and lifestyle factors before prescribing medications that may potentially contribute to DVT.
Patient education is equally important in preventing DVT associated with medications. Individuals should be informed about the potential risks of their prescribed medications and encouraged to communicate any unusual symptoms to their healthcare providers promptly. Regular check-ups, monitoring, and adjustments to medication regimens as needed are essential components of managing the risk of DVT in patients taking medications that may impact coagulation.
In conclusion, while medications are vital tools in managing various health conditions, a thorough understanding of their potential side effects, including their influence on the risk of DVT, is crucial for both healthcare providers and patients. A collaborative and informed approach to medication management can help mitigate risks and ensure the overall well-being of individuals requiring pharmacological interventions for their health conditions.