How To Reverse Insulin Resistance Quickly
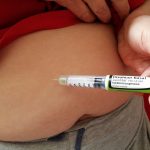
Human insulin is a protein derived from a 74-amino-acid prohormone molecule called proinsulin. It is used to control blood sugar in people who have type 1 diabetes (a condition in which the body does not make insulin and therefore cannot control the amount of sugar in the blood) or in people who have type 2 diabetes (a condition in which the blood sugar is too high because the body does not produce or use insulin normally) that cannot be controlled with oral medications alone. Human insulin is in a class of medications called hormones. Human insulin is used to take the place of insulin that is normally produced by the body. It works by helping move sugar from the blood into other body tissues where it is used for energy. It also stops the liver from producing more sugar. All of the types of insulin that are available work in this way. The types of insulin differ only in how quickly they begin to work and how long they continue to control blood sugar.
What Is Insulin Resistance?
Insulin resistance is when cells in your muscles, fat, and liver don’t respond well to insulin and can’t use glucose from your blood for energy. To make up for it, your pancreas makes more insulin. Over time, your blood sugar levels go up. This increases the risk of developing prediabetes and, eventually, type 2 diabetes. If the pancreas can make enough insulin to overcome the low rate of absorption, diabetes is less likely to develop, and blood glucose will stay within a healthy range. Insulin resistance affects as many as 1 in 3 Americans. You might also hear it called metabolic syndrome.
What are the symptoms of insulin resistance?
There are usually no symptoms of insulin resistance in the early stages. Over time, the combined high blood glucose, high insulin levels, and insulin resistance can lead to complications in multiple body systems.
The symptoms a person experiences will largely depend on the underlying cause of insulin resistance in their body and the complications that develop.
Some people with insulin resistance may have one or more of these subtle signs:
• Irregular menstrual cycle
• Hirsutism (excessive body hair)
• Acanthosis nigricans (thick, dark patches of skin in skin folds or creases)
Insulin resistance syndrome includes a group of problems like obesity, high blood pressure, high cholesterol, and type 2 diabetes. If you have experienced any of these symptoms, speak with a healthcare provider to determine if you need to be checked for signs of insulin resistance.
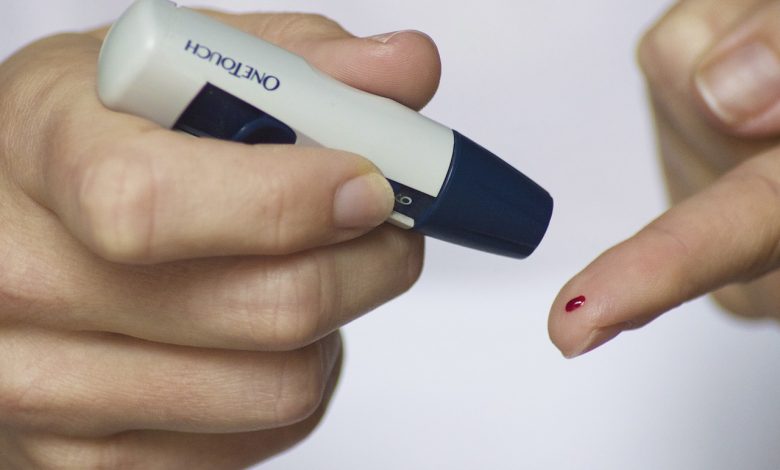
In clinical practice, no single laboratory test is used to diagnose insulin resistance syndrome. Diagnosis is based on clinical findings corroborated with laboratory tests. Individual patients are screened based on the presence of comorbid conditions. Laboratory tests include the plasma glucose level, the fasting insulin level, and a lipid profile, among others.
How to reverse Insulin resistance
Treatment involves pharmacologic therapy to reduce insulin resistance, along with surgical management of underlying causes if appropriate. Comorbid conditions should be evaluated and addressed; this is generally feasible on an outpatient basis, though some patients will require admission. The metabolic syndrome requires aggressive control of cardiovascular and metabolic risk factors. Modifications of diet and activity are recommended. Medications that reduce insulin resistance (insulin-sensitizing and antihyperglycemic effects) include metformin and thiazolidinediones.
In addition, you can take some steps to reduce the likelihood of developing insulin resistance. Some of the same strategies, such as managing weight or quitting smoking, are key to preventing heart disease and stroke. Experts say that up to 50% of people with prediabetes can prevent the onset of diabetes through such measures.
According to the CDC, if an overweight or obese person loses 5–7% of their body weight, it can significantly reduce their risk of developing diabetes. Regular exercise can also help. Muscles become more sensitive to insulin after exercise, helping the body reverse insulin resistance.
How to use diet to reverse insulin resistance
According to the Centers For Disease Control and Prevention, lifestyle changes can help improve insulin sensitivity and even reverse the effects of insulin resistance. Carefully choosing what you include in your diet is an important way to help with insulin resistance and avoid high blood sugar. The American Diabetes Association (ADA) often recommends talking with a professional like a dietician to improve your diet if you have prediabetes or diabetes.
High-protein, low-carbohydrate diets are recommended because protein helps keep your body’s blood glucose levels stable. High-carbohydrate diets can cause spikes in blood glucose levels that only make insulin resistance worse. Being insulin resistant doesn’t necessarily mean you have diabetes, but following a meal plan recommended by the ADA can help improve insulin sensitivity.
High protein, low-sugar foods to eat for a reduced-insulin-resistance, low-carb diet include:
• Low-fat dairy products (low-fat yogurt, low-fat cheese)
• Meats and poultry (chicken, fish, and eggs)
• Nuts
• Vegetables
• Whole grains
A diagnosis of insulin resistance can be worrying, but it is not necessarily too late to prevent diabetes.