Empathetic Remarks By Doctors to Patients Can Reduce Pain – Study
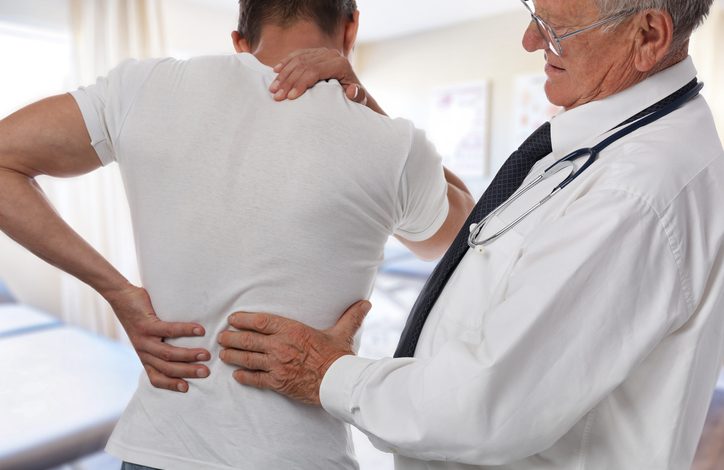
Physicians’ displays of empathy towards their patients have been shown to reduce the sensation of pain, according to a recent study published in the Proceedings of the National Academy of Sciences. The research, conducted by a team led by neuroscientist Dan-Mikael Ellingsen, Ph.D., from Oslo University Hospital in Norway, utilized functional MRI (fMRI) to scan the brains of 20 patients suffering from chronic pain. The goal was to investigate how a physician’s demeanor might impact patients’ sensitivity to pain, particularly within the central nervous system.
During the study, the patient’s legs were exposed to stimuli of varying intensities, ranging from painless to moderately painful. Using a pain intensity scale, the patients reported their perceived pain levels during the scans. The physicians themselves also underwent fMRI.
The study was divided into different conditions. Half of the patients experienced the pain stimuli alone, while the other half experienced it in the presence of a physician. The latter group was further divided into two subgroups: one subgroup interacted with the accompanying physician before the examination, discussing their medical history and condition, while the other subgroup had no prior interaction with the physician before the brain scans.
The results showed that patients who had a physician present during the examination reported less pain compared to those who were alone, even when subjected to stimuli of the same intensity. Notably, patients who had spoken to the physician before the brain scan felt that the physician was empathetic and understood their pain better. Additionally, the physicians were more accurate in estimating the pain intensity experienced by their patients if they had established a prior connection.
The brain scans revealed that patients who had interacted with a physician showed increased activity in specific brain regions, including the dorsolateral and ventrolateral prefrontal cortex, as well as in the primary and secondary somatosensory areas. These brain areas are known to be involved in processing pain signals. For physicians, there was a higher correlation between activity in the dorsolateral prefrontal cortex and activity in the secondary somatosensory areas of patients they had spoken to. This correlation was related to the level of mutual trust reported by the physician and patient.

Adjunct Prof Winfried Meißner, MD, who heads the pain clinic at the Department of Anesthesiology and Intensive Care Medicine at Jena University Hospital in Germany and is the former president of the German Pain Society, praised the study as a crucial piece of evidence highlighting the importance of effective pain therapy beyond simply administering the correct analgesic.
He emphasized that an empathetic attitude from physicians and good communication with patients play a vital role in the success of any pain therapy. Unfortunately, in clinical practice, time constraints often hinder the provision of such empathetic communication.
With the objectively collected data from both patients and physicians, the study led by Dan-Mikael Ellingsen’s team demonstrates the decisive impact of human interaction on the treatment of patients experiencing pain. This finding should encourage healthcare practitioners to take communication as seriously as the use of pharmacological interventions in pain management.
Meißner highlighted that empathetic conversations between physicians and patients should be recognized as a valuable therapeutic method, which can complement and strengthen pharmacological treatments. While conversation cannot replace medication, it can have an equally significant effect on patients’ perception of pain, making it more than just a sensory experience.
He also stressed the importance of positive expectations in pain management. Studies have shown that a patient’s positive expectations can enhance the effectiveness of medications. Therefore, physicians should take into account the psychological factors influencing pain perception and use this knowledge to optimize treatment outcomes.
Meißner advises all physicians to approach patients with pain empathetically and to inquire about not only their physical symptoms but also their accompanying emotions, fears, and mental stress. By addressing these aspects, healthcare providers can contribute to a more holistic and effective pain management approach.