Drug-Induced Parkinsonism Treatment Drugs

What is drug-induced parkinsonism?
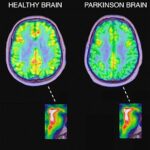
About 7% of people with parkinsonism have developed their symptoms following treatment with particular medications. This form of parkinsonism is called ‘drug-induced parkinsonism’. People with idiopathic Parkinson’s disease and other causes of parkinsonism may also develop worsening symptoms if treated with such medication inadvertently.
What drugs cause drug-induced parkinsonism?
Any drug that blocks the action of dopamine (referred to as a dopamine antagonist) is likely to cause parkinsonism. Drugs used to treat schizophrenia and other psychotic disorders such as behaviour disturbances in people with dementia (known as neuroleptic drugs) are possibly the major cause of drug-induced parkinsonism worldwide.
Parkinsonism can occur from the use of any of the various classes of neuroleptics. The atypical neuroleptics – clozapine (Clozaril) and quetiapine (Seroquel), and to a lesser extent olanzapine (Zyprexa) and risperidone (Risperdal) – appear to have a lower incidence of extrapyramidal side effects, including parkinsonism. These drugs are generally best avoided by people with Parkinson’s, although some may be used by specialists to treat symptoms such as hallucinations occurring with Parkinson’s. Risperidone and olanzapine should be used with caution to treat dementia in people at risk of stroke (the risk increases with age, hypertension, diabetes, atrial fibrillation, smoking and high cholesterol), because of an increased risk of stroke and other cerebrovascular problems. It is unclear whether there is an increased risk of stroke with quetiapine and clozapine.
While these drugs are used primarily as antipsychotic agents, it is important to note that they can be used for other non-psychiatric uses, such as control of nausea and vomiting. For people with Parkinson’s, other anti-sickness drugs such as domperidone (Motilium) or ondansetron (Zofran) would be preferable. As well as neuroleptics, some other drugs can cause drug-induced parkinsonism. These include some older drugs used to treat high blood pressure such as methyldopa (Aldomet); medications for dizziness and nausea such as prochlorperazine (Stemetil); and metoclopromide (Maxolon), which is used to stop sickness and in the treatment of indigestion.
Calcium channel blocking drugs used to treat high blood pressure, abnormal heart rhythm, angina pectoris, panic attacks, manic depression and migraine may occasionally cause drug-induced parkinsonism. The most well-documented are cinnarizine (Stugeron) and flunarizine (Sibelium). Calcium channel blocking drugs are, however, widely used to treat angina and high blood pressure, and it is important to note that most common agents in clinical use probably do not have this side effect. These drugs should never be stopped abruptly without discussion with your doctor.
A number of other agents have been reported to cause drug-induced parkinsonism, but clear proof of cause and effect is often lacking. Amiodarone, used to treat heart problems, causes tremor and some people have been reported to develop Parkinson’s-like symptoms. Sodium valproate, used to treat epilepsy, and lithium, used in depression, both commonly cause tremor which may be mistaken for Parkinson’s. Some reports have linked SSRI antidepressant drugs such as fluoxetine (Prozac) to drug-induced parkinsonism but hard evidence of cause and effect is unsubstantiated. This type of drug is increasingly used to treat depression in Parkinson’s.
What are neuroleptic drugs?
An estimated 60% of Parkinson’s patients will experience some form of psychosis during their illness, according to a study. Neuroleptics, also known as antipsychotic medications, are medications that are used to treat schizophrenia and other psychotic disorders. They work by blocking dopamine receptors in the nervous system.
There are two classes of neuroleptic drugs: the “typical,” also known as “first-generation,” drugs and the more commonly prescribed “atypical”, or “second-generation,” drugs. First-generation neuroleptics are further categorized as high or low potency, based on the amount of the drug required to minimize the symptoms. Common high-potency, first-generation neuroleptics include haloperidol, trifluoperazine, and fluphenazine. Common low-potency, first-generation neuroleptics include thioridazine, chlorpromazine, and thiothixene. Among second-generation medications, clozapine, olanzapine, paliperidone, and risperidone are the most frequently prescribed.