Can Antibiotics Cause Mouth Thrush?
Antibiotics have undoubtedly revolutionized modern medicine, saving countless lives by combating bacterial infections. However, their use is not without consequences, and one such consequence that often raises concern is the development of oral thrush.
This article explores the relationship between antibiotics and mouth thrush, delving into the mechanisms at play, the risk factors involved, and strategies to mitigate the occurrence of this common oral infection.
Understanding Antibiotics
Antibiotics are medications designed to kill or inhibit the growth of bacteria. They play a crucial role in treating bacterial infections ranging from common respiratory illnesses to more severe conditions like pneumonia and urinary tract infections. While antibiotics are essential in managing bacterial infections, their use can have unintended consequences on the delicate balance of microorganisms within the body, particularly in the oral cavity.
The Oral Microbiome
The human mouth is a complex ecosystem inhabited by a diverse array of microorganisms, including bacteria, fungi, and viruses. The balance of these microorganisms is essential for maintaining oral health. Disruption of this balance can lead to overgrowth of certain microorganisms, creating an environment conducive to infections such as oral thrush.
Mouth Thrush: A Fungal Overgrowth
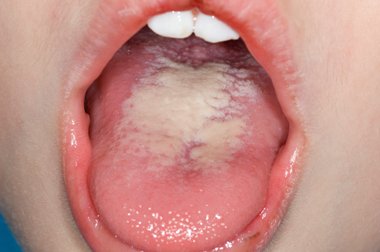
Oral thrush, scientifically known as candidiasis, is a fungal infection caused by the overgrowth of Candida species, primarily Candida albicans, in the mouth. Candida is a naturally occurring fungus present in the oral cavity, gastrointestinal tract, and other mucosal surfaces. Under normal circumstances, the immune system and the balance of microorganisms prevent Candida from proliferating excessively. However, when this delicate balance is disrupted Candida can multiply, leading to the development of oral thrush.
Symptoms of oral thrush
In its early stages, oral thrush may not cause any symptoms. But as the infection gets worse, one or more of the following symptoms may develop:
• white or yellow spots on your inner cheeks, tongue, tonsils, gums, or lips
• slight bleeding if the spots are scraped
• soreness or burning in your mouth
• a cotton-like sensation in your mouth
• dry, cracked skin at the corners of your mouth
• difficulty swallowing
• a bad taste in your mouth
• a loss of taste
• redness, irritation, and pain under dentures (denture stomatitis)
In some cases, oral thrush can affect your esophagus, though this is uncommon. The same fungus that causes oral thrush can also cause yeast infections in other parts of your body.
Can Antibiotics Cause Mouth Thrush?
Yes, antibiotics can contribute to the development of mouth thrush. The connection between antibiotics and oral thrush lies in the disruption of the natural balance of microorganisms within the oral cavity, particularly the overgrowth of Candida species, primarily Candida albicans.
Antibiotics are medications designed to combat bacterial infections by either killing or inhibiting the growth of bacteria. While they are effective in treating bacterial infections, their action is not specific, and they can also impact beneficial bacteria in the body. This indiscriminate effect on the microbiome can create an environment conducive to the overgrowth of opportunistic fungi, such as Candida.
Several mechanisms explain how antibiotics contribute to the development of oral thrush:
1. Disruption of Microbial Balance: Antibiotics are designed to target a broad spectrum of bacteria, both harmful and beneficial. This broad-spectrum action can disrupt the delicate balance of microorganisms in the oral cavity, leading to an environment where Candida can proliferate.
2. Suppression of Immune Response: Some antibiotics may affect the immune system’s ability to regulate fungal overgrowth. A compromised immune response can increase susceptibility to infections like oral thrush.
3. Broad-Spectrum Antibiotics: Certain classes of antibiotics, known as broad-spectrum antibiotics, target a wide range of bacteria. While effective against bacterial infections, these antibiotics can have a more pronounced impact on the oral microbiome, increasing the risk of fungal overgrowth.
4. Prolonged or Repeated Use: The duration and frequency of antibiotic use are critical factors. Prolonged or repeated courses of antibiotics can disrupt the microbial balance for an extended period, allowing Candida to establish persistent infections.
It is important to note that while antibiotics are a common risk factor for oral thrush, other factors can also contribute, including weakened immune function, underlying health conditions, poor oral hygiene, and the use of certain medications.
Mitigating the Risk
1. Probiotics: Probiotics, beneficial bacteria that promote a healthy microbial balance, can be a proactive measure to mitigate the risk of oral thrush during and after antibiotic treatment. Incorporating probiotic-rich foods or supplements helps restore the balance of microorganisms in the oral cavity and gastrointestinal tract.
2. Oral Hygiene Practices: Maintaining good oral hygiene is crucial in preventing oral thrush. Regular brushing, flossing, and the use of antiseptic mouthwashes help control the growth of microorganisms and reduce the risk of fungal overgrowth.
3. Limited and Informed Antibiotic Use: Healthcare professionals play a pivotal role in minimizing the risk of oral thrush associated with antibiotic use. Prescribing antibiotics judiciously, considering the specific microbial target, and informing patients about the potential risks can contribute to more responsible antibiotic use.
4. Monitoring and Early Intervention: Close monitoring of patients undergoing antibiotic treatment allows healthcare providers to detect early signs of fungal overgrowth. Timely intervention, such as adjusting the antibiotic regimen or introducing antifungal medications, can help prevent the progression of oral thrush.
Conclusion
The relationship between antibiotics and mouth thrush underscores the intricate interplay within the human body’s microbiome. While antibiotics are indispensable in treating bacterial infections, their impact on the delicate balance of microorganisms requires careful consideration. Healthcare professionals and patients alike must be aware of the risks associated with antibiotic use and work collaboratively to implement strategies that mitigate these risks. By embracing responsible antibiotic practices, incorporating preventive measures, and staying vigilant in monitoring patients, it is possible to strike a balance between effective infection management and the preservation of overall oral health.