What are the Common Side Effects Of Anti TB Drugs
Tuberculosis (TB) is a bacterial infection spread through inhaling tiny droplets from the coughs or sneezes of an infected person. It mainly affects the lungs, but it can affect any part of the body, including the tummy (abdomen), glands, bones and nervous system.
In the past, TB was a major cause of death around the world. Following improvements in living conditions and the development of antibiotics, the prevalence of TB fell dramatically in industrialized countries.
However, in the 1980s, numbers started to rise again. The World Health Organization (WHO) describe it as an “epidemic.” They report that it is among the top 10 causes of death globally and “the leading cause of death from a single infectious agent.” The WHO estimate that in 2018, nearly 10 million people around the world developed TB and 1.5 million people died from the disease, including 251,000 people who also had HIV. A majority of the people affected were in Asia. However, TB remains a matter of concern in many other areas, including the United States.
The same year, doctors reported 9,025 cases of TB in the U.S., according to the Centers for Disease Control and Prevention (CDC). Currently, antibiotic resistance is causing renewed concerns about TB among experts. Some strains of the disease are not responding to the most effective treatment options. In this case, TB is difficult to treat.
How is TB Treated?
It is very important that people who have TB disease are treated, finish the medicine, and take the drugs exactly as prescribed. If they stop taking the drugs too soon, they can become sick again; if they do not take the drugs correctly, the TB bacteria that are still alive may become resistant to those drugs. TB that is resistant to drugs is harder and more expensive to treat.
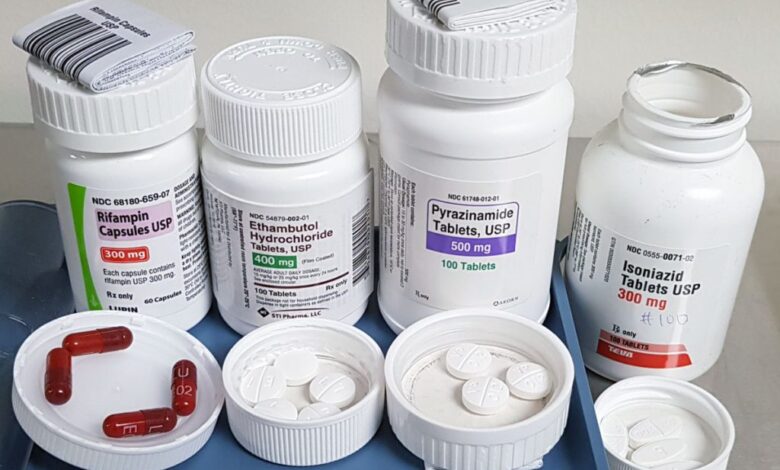
TB disease can be treated by taking several drugs for 6 to 9 months. There are 10 drugs currently approved by the U.S. Food and Drug Administration (FDA) for treating TB. Of the approved drugs, the first-line anti-TB agents that form the core of treatment regimens are:
- isoniazid (INH)
- rifampin (RIF)
- ethambutol (EMB)
- pyrazinamide (PZA)
What are the common side effects of anti TB drugs?
The common side effects of TB drugs include:
- feeling sick or dizzy
- skin rashes
- pins and needles
- flu like symptoms
In very few cases, people may experience jaundice, which is the yellowing of skin or eyes. If this happens, stop taking your medication and tell your doctor straight away.
The common side effects of individual TB medications is presented below:
Isoniazid: Common side effects of isoniazid include:
- numbness and tingling in the extremities,
- hepatitis (symptoms include loss of appetite, nausea, vomiting, fatigue, malaise, and weakness),
- nausea,
- vomiting,
- upset stomach,
- fever,
- rash.
Rifampin: common side effects of rifampin include:
- heartburn.
- abdominal pain.
- loss of appetite.
- nausea.
- vomiting.
- yellowing skin and eyes (jaundice)
- gas (flatulence)
- cramps.
Ethambutol: common side effects of ethambutol may include:
- itching or rash;
- joint pain;
- headache, dizziness; or.
- nausea, vomiting, stomach pain, indigestion, loss of appetite.
Pyrazinamide: common side effects of pyrazinamide include:
- nausea,
- upset stomach,
- vomiting,
- loss of appetite,
- mild muscle or joint pain, or.
- fatigue.
Managing the side effects of medication is important in helping people to complete their TB treatment. This is crucial to minimize the impact of TB on a person’s health and to stop them spreading the illness.
The side effects of TB drugs depend on the treatment. These range from mild but annoying to severe, and can sometimes even warrant a change of medication. Dealing with side effects during at least six months of treatment can prove very challenging for people, and is another thing to contend with along with symptoms of the illness itself.
In general, the first line drugs used to treat drug-sensitive TB are better tolerated than the second line medications for drug-resistant TB.

