7 Things You Should Know About Amoxicillin Rash (Pictures)
The discovery of penicillin by Alexander Fleming in 1928 marked a groundbreaking advancement in medicine, revolutionizing the treatment of bacterial infections. However, as penicillin and its derivatives became more widely used, reports of allergic reactions began to surface. The earliest documented cases of penicillin allergy date back to the 1940s, shortly after the widespread clinical use of penicillin during World War II.
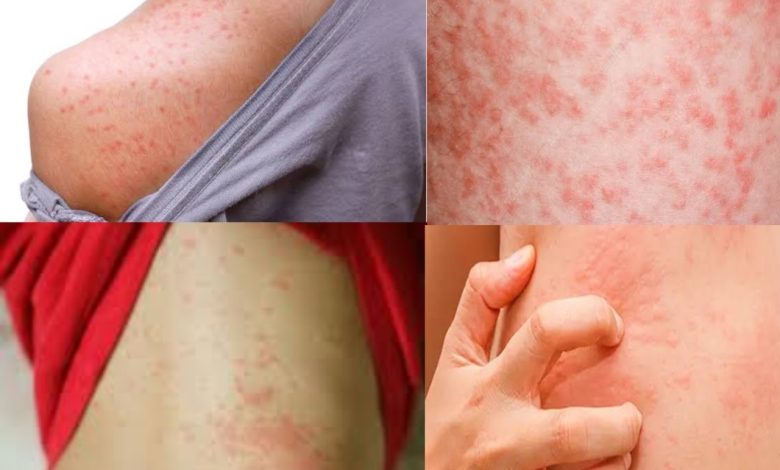
As penicillin and its derivatives evolved, including amoxicillin, reports of allergic reactions, including rashes, became more prevalent. The amoxicillin rash, characterized by red or pink spots on the skin, was identified as a common adverse reaction to this antibiotic, particularly in children.
One of the earliest documented cases of an amoxicillin rash may have occurred in the late 20th century as amoxicillin gained popularity as a broad-spectrum antibiotic. Medical literature from the 1970s onwards began to document cases of allergic reactions, including rashes, associated with amoxicillin and other penicillin antibiotics.
Since then, numerous case reports, clinical studies, and reviews have described the characteristics, management, and outcomes of amoxicillin rash. These studies have contributed to our understanding of the immunological mechanisms underlying allergic reactions to penicillin antibiotics and have helped healthcare professionals recognize and manage these adverse events more effectively.
What is amoxicillin rash?
Amoxicillin rash refers to a skin reaction that occurs as a side effect of taking amoxicillin, which is a commonly prescribed antibiotic. It is one of the most frequently reported adverse reactions to amoxicillin and other penicillin-based antibiotics. This rash typically appears as red or pink spots on the skin and may be accompanied by itching or discomfort. In some cases, the rash may be more widespread and resemble hives or small, raised bumps.
The exact mechanism underlying the development of an amoxicillin rash is not fully understood, but it is believed to be an immune-mediated reaction. When exposed to amoxicillin, certain individuals may have an allergic response, leading to the release of histamines and other inflammatory substances in the body. This immune response results in the characteristic rash.
Amoxicillin rash usually occurs within a few days to weeks after starting the medication. It can occur in both children and adults, but it is more common in children. The rash typically resolves on its own within a few days after discontinuation of the antibiotic. However, in some cases, it may persist or worsen, requiring medical attention.
It’s important to distinguish between an amoxicillin rash and a more serious allergic reaction known as anaphylaxis. Anaphylaxis is a severe and potentially life-threatening allergic reaction that can cause difficulty breathing, swelling of the face or throat, rapid heartbeat, and a drop in blood pressure. If any of these symptoms occur after taking amoxicillin, immediate medical attention is necessary.
Risk Factors
Developing an Amoxicillin Rash can be influenced by several factors. Understanding these risk factors is crucial for both patients and healthcare providers to recognize and manage potential allergic reactions effectively.
1. Previous allergic reactions to penicillin or other beta-lactam antibiotics: Individuals with a history of hypersensitivity reactions to penicillin or other antibiotics within the beta-lactam class are at an increased risk of developing an allergic reaction to amoxicillin. This heightened sensitivity may result in the manifestation of a rash upon exposure to the drug.
2. History of asthma, hay fever, or other allergic conditions: Patients with pre-existing allergic conditions, such as asthma or hay fever, may have a heightened immune response to certain allergens, including antibiotics like amoxicillin. The presence of underlying allergic conditions can predispose individuals to develop allergic reactions, including skin rashes when exposed to triggering agents.
3. Genetic predisposition to allergic reactions: Genetic factors play a significant role in determining an individual’s susceptibility to allergic reactions. Certain genetic variations can influence the immune system’s response to foreign substances, increasing the likelihood of developing allergic responses to medications like amoxicillin.
4. Concurrent viral infections, such as infectious mononucleosis: Viral infections, particularly infectious mononucleosis caused by the Epstein-Barr virus, can influence the body’s immune response and increase the risk of developing an allergic reaction to antibiotics like amoxicillin. The presence of viral infections can exacerbate the likelihood of developing a rash when taking certain medications.
Symptoms
Recognizing the symptoms associated with an Amoxicillin Rash in adults and children is essential for prompt diagnosis and management. While the rash typically manifests within a few days to weeks after initiating amoxicillin treatment, it may vary in presentation and severity among individuals. Common symptoms include:
1. Red or pink spots on the skin: The rash may appear as small, red or pink spots scattered across the skin surface. These spots can vary in size and may be accompanied by other features such as swelling or inflammation.
2. Rash that may be flat or raised: The rash can present as either flat or raised lesions on the skin. It may have a smooth texture or appear bumpy, depending on the individual’s reaction to the medication.
3. Itching or discomfort: Many patients with an Amoxicillin Rash experience itching or discomfort associated with the rash. The sensation of itching can range from mild to severe and may interfere with daily activities and quality of life.
4. Occasionally, the rash may be accompanied by other symptoms: In some cases, the rash may be accompanied by additional symptoms such as fever, swelling, or joint pain. These systemic manifestations may indicate a more severe allergic reaction requiring immediate medical attention.
Diagnosis
Accurate diagnosis of an Amoxicillin Rash relies on a comprehensive evaluation of clinical features, medical history, and, in some cases, diagnostic tests. Key aspects of the diagnostic process include:
1. Medical history: Healthcare providers will inquire about the patient’s medical history, including any previous allergic reactions to medications, particularly penicillin or other beta-lactam antibiotics.
2. Physical examination: A thorough examination of the skin is essential to assess the characteristics of the rash, including its distribution, morphology, and associated symptoms. Additionally, healthcare providers will evaluate for any signs of systemic involvement, such as fever or swelling.
3. Timing of the rash in relation to antibiotic use: Establishing the temporal relationship between the onset of the rash and initiation of amoxicillin therapy is critical. A rash that develops shortly after starting the medication is highly suggestive of an allergic reaction.
4. Additional tests: In certain cases, healthcare providers may recommend additional tests to confirm the diagnosis of an Amoxicillin Rash. These may include skin prick testing, patch testing, or blood tests to assess for specific antibodies associated with allergic reactions.
Management
Effectively managing an Amoxicillin Rash involves a multifaceted approach aimed at alleviating symptoms, preventing complications, and ensuring optimal patient outcomes. Key management strategies include:
1. Discontinuation of the offending antibiotic: Prompt discontinuation of amoxicillin is essential upon suspicion of an allergic reaction. Stopping the medication helps prevent further exposure and mitigate the risk of worsening symptoms or complications.
2. Symptomatic treatment: Over-the-counter antihistamines, such as diphenhydramine or loratadine, can help alleviate itching and discomfort associated with the rash. Additionally, topical corticosteroids, such as hydrocortisone cream, may provide relief from inflammation and irritation.
3. Monitoring: Patients should be closely monitored for any signs of worsening symptoms or development of systemic complications. Healthcare providers should assess for symptoms of anaphylaxis, such as difficulty breathing, swelling of the face or throat, and lightheadedness, which require immediate medical attention.
4. Alternative antibiotics: In cases where antibiotic therapy is necessary, alternative agents that are structurally distinct from penicillins, such as macrolides or cephalosporins, may be considered. Healthcare providers should select alternative antibiotics based on the underlying infection, antibiotic susceptibility patterns, and the patient’s individual factors.
Prognosis
The prognosis of an Amoxicillin Rash is generally favorable, with most cases resolving spontaneously upon discontinuation of the offending medication. However, in rare instances, the rash may progress to more severe allergic reactions, such as anaphylaxis, which can be life-threatening if not promptly treated.
Close monitoring and appropriate management are essential to ensure a favorable outcome and prevent complications. Patients should be educated about the importance of avoiding amoxicillin and related antibiotics in the future to prevent the recurrence of allergic reactions.
Conclusion
The Amoxicillin Rash represents a common adverse reaction to this widely prescribed antibiotic. While typically benign, it underscores the importance of vigilant monitoring and judicious use of antibiotics in clinical practice. Healthcare providers play a crucial role in recognizing and managing allergic reactions effectively, ensuring optimal patient care and safety.
By understanding the risk factors, symptoms, diagnostic approach, and management strategies associated with an Amoxicillin Rash, healthcare providers can confidently navigate the complexities of antibiotic therapy and minimize the risk of adverse outcomes. Through comprehensive patient education and proactive management, the incidence and impact of allergic reactions to antibiotics can be mitigated, ultimately enhancing patient well-being and treatment outcomes.