10 Effective Treatments For Bumps On Vaginal Area
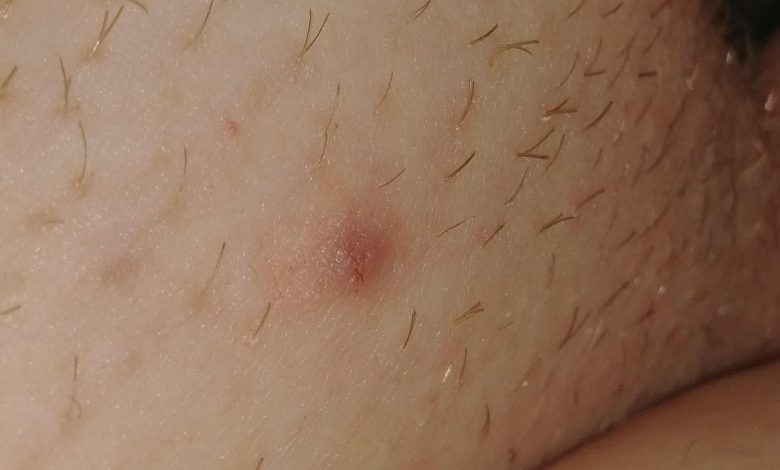
Bumps on the vaginal area can have various causes and may not always be a cause for concern. Here are the potential causes of bumps in the vaginal area:
- Ingrown hairs: Shaving or waxing the pubic area can sometimes lead to ingrown hairs, which are hairs that curl and grow back into the skin. These can appear as small, red bumps and may be accompanied by itching or discomfort.
- Razor burn or irritation: Irritation from shaving, using harsh soaps, or wearing tight clothing can cause redness and bumps in the vaginal area. Ensuring proper hygiene, using gentle cleansers, and wearing loose-fitting clothing can help prevent this.
- Folliculitis: This is an infection or inflammation of the hair follicles, which can occur due to bacteria, yeast, or friction. It can manifest as small, red, and tender bumps around the hair follicles.
- Genital herpes: Herpes is a sexually transmitted infection (STI) caused by the herpes simplex virus (HSV). It can lead to the formation of small, painful blisters or sores in the genital area.
- Genital warts: Caused by certain strains of the human papillomavirus (HPV), genital warts are typically soft, flesh-colored growths that can appear in the vaginal area.
- Bartholin’s cyst: The Bartholin’s glands are located on either side of the vaginal opening. If the ducts of these glands become blocked, fluid can accumulate and form a cyst, resulting in a painless lump in the vaginal area.
What medications are effective for bumps on the vaginal area?
The specific medications used to treat bumps on the vaginal area depend on the underlying cause of the bumps. Here are some common medications that healthcare professionals may recommend for certain conditions:
1. Antiviral medications: If the bumps are caused by a viral infection, such as genital herpes, antiviral medications like acyclovir, valacyclovir, or famciclovir may be prescribed to reduce the severity and duration of outbreaks. Examples of antiviral medications used for herpes include:
• Acyclovir (Zovirax)
• Valacyclovir (Valtrex)
• Famciclovir (Famvir)
These medications can help reduce the severity and duration of outbreaks and may be prescribed in oral form.
2. Topical antibiotics: If the bumps are due to a bacterial infection, a healthcare professional may prescribe topical antibiotics, such as mupirocin or clindamycin, to treat the infection and reduce inflammation. Examples of topical antibiotics used for bacterial infections include:
• Mupirocin (Bactroban)
• Clindamycin (Cleocin)
These medications are typically applied directly to the affected area in the form of creams or ointments.
3. Antifungal medications: For fungal infections, such as yeast infections, antifungal medications like clotrimazole, miconazole, or fluconazole may be recommended in the form of topical creams, suppositories, or oral tablets. Examples of antifungal medications used for yeast infections include:
• Clotrimazole (Gyne-Lotrimin)
• Miconazole (Monistat)
• Fluconazole (Diflucan)
These medications can be available as topical creams, suppositories, or oral tablets.
4. Corticosteroids: In cases where bumps are caused by inflammatory conditions like contact dermatitis or lichen sclerosus, a healthcare professional may prescribe topical corticosteroids to reduce inflammation, itching, and discomfort.
Examples of topical corticosteroids include:
• Hydrocortisone cream
• Triamcinolone acetonide cream (Kenalog)
These medications are applied directly to the affected area and should be used under the guidance of a healthcare professional.
5. Local anesthetics: For bumps that are causing significant pain or discomfort, a healthcare professional may suggest the use of local anesthetics, such as lidocaine ointment or cream, to temporarily numb the area.
6. Antihistamines: If the bumps are caused by an allergic reaction or histamine release, antihistamine medications may be recommended to reduce itching and inflammation. Examples of antihistamines include:
• Diphenhydramine (Benadryl)
• Cetirizine (Zyrtec)
• Loratadine (Claritin)
These medications are available in oral form and can help alleviate symptoms associated with allergic reactions.
7. Immunomodulators: In certain cases, when bumps on the vaginal area are related to chronic skin conditions like lichen planus or lichen sclerosus, immunomodulator medications may be prescribed. Examples of immunomodulators include:
• Tacrolimus ointment (Protopic)
• Pimecrolimus cream (Elidel)
These medications work by modulating the immune response in the affected area and reducing inflammation.
8. Analgesics: If the bumps are causing significant pain or discomfort, over-the-counter analgesics or pain relievers may be used to alleviate symptoms. Examples of analgesics include:
• Acetaminophen (Tylenol)
• Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) or naproxen (Aleve)
These medications can help reduce pain and inflammation, but it’s important to follow the recommended dosage and consult a healthcare professional if you have any underlying medical conditions.
9. Vaginal creams or gels: Depending on the specific diagnosis, healthcare professionals may recommend specific vaginal creams or gels that contain active ingredients to address the underlying cause of the bumps. These may include:
• Estrogen creams for certain conditions like vaginal atrophy or lichen sclerosus
• Anti-inflammatory creams with ingredients like hydrocortisone for inflammation or irritation
These medications are typically applied directly to the affected area and should be used as directed by a healthcare professional.
It’s important to note that the appropriate medication and treatment approach will depend on the underlying cause of the bumps. It’s crucial to consult with a healthcare professional for an accurate diagnosis and personalized treatment recommendations based on your specific situation. They will be able to provide you with the most appropriate medications and guide you through the treatment process.
It’s important to consult with a healthcare professional, such as a gynecologist or dermatologist, for an accurate diagnosis and appropriate treatment. They will be able to evaluate your specific situation, determine the underlying cause of the bumps, and recommend the most effective medications or treatments tailored to your needs.
Non Medicinal Treatment For Bumps On the Vaginal Area
In addition to medications, there are non-medicinal treatments and self-care measures that can help alleviate discomfort and promote healing for bumps on the vaginal area. Here are some non-medicinal treatment options:
1. Warm water baths: Soaking in a warm bath can help soothe the affected area and provide temporary relief from itching or discomfort. Avoid using harsh soaps or bath products that may irritate the skin further.
2. Gentle cleansing: Clean the affected area gently with mild, fragrance-free soap and warm water. Avoid excessive scrubbing or using harsh cleansers that can further irritate the skin. Pat the area dry with a clean towel, avoiding rubbing.
3. Cool compresses: Applying a cool compress or ice pack wrapped in a clean cloth to the affected area can help reduce inflammation and provide temporary relief from pain or itching.
4. Loose-fitting clothing: Wear loose-fitting, breathable cotton underwear and avoid tight clothing that may cause friction and further irritation. This allows for better airflow and helps keep the area dry.
5. Avoid irritants: Identify and avoid potential irritants that may worsen symptoms. This may include scented feminine hygiene products, perfumed soaps, bubble baths, and harsh detergents.
6. Sitz baths: A sitz bath is a shallow bath that covers the hips and buttocks area. You can use a specialized sitz bath basin or a clean bathtub filled with warm water. Soaking in a sitz bath for 10 to 15 minutes a few times a day can help reduce inflammation and promote healing.
7. Avoid scratching: Although it may be tempting, avoid scratching the affected area, as it can lead to further irritation, inflammation, and potential infection. If necessary, consider using clean, damp cotton pads to gently dab or pat the area instead of scratching.
8. Stress reduction: Stress can worsen symptoms and delay healing. Engage in stress-reducing activities such as deep breathing exercises, meditation, yoga, or gentle exercise to promote relaxation and support overall well-being.
It’s important to note that these non-medicinal treatments can provide symptomatic relief and support healing, but they may not address the underlying cause of the bumps. If the bumps persist, worsen, or are accompanied by concerning symptoms, it’s crucial to consult a healthcare professional for a proper diagnosis and appropriate treatment.

