How Antidepressant Response is Measured
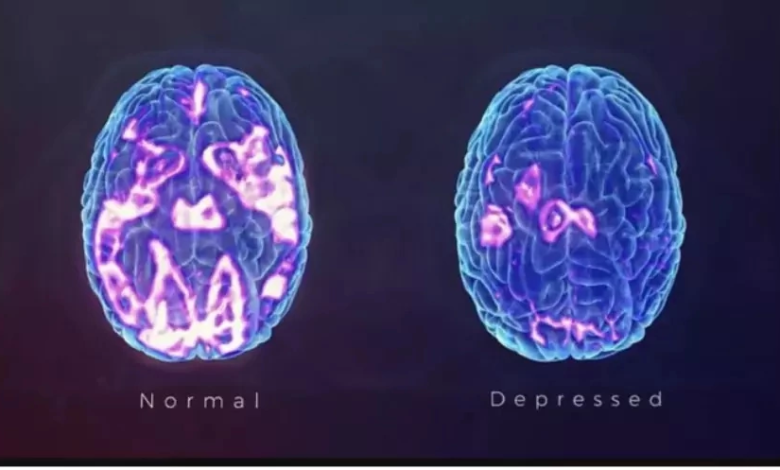
Antidepressant response refers to the degree of improvement in a person’s mood and overall mental well-being when they are treated with antidepressant medications. These medications are primarily prescribed to individuals experiencing symptoms of depression, which can include persistent sadness, lack of interest or pleasure in activities, changes in appetite or sleep patterns, feelings of worthlessness, and difficulty concentrating. The goal of antidepressant treatment is to alleviate these symptoms and help individuals regain a sense of emotional equilibrium and functioning in their daily lives.
The effectiveness of antidepressant response can vary from person to person. Some individuals may experience significant relief from their depressive symptoms within a few weeks of starting medication, while others may require several months or need to try different medications before finding one that works for them. Factors such as the type of antidepressant prescribed, the severity of the depression, and an individual’s unique biology can all influence the degree of response to treatment. It’s important for individuals undergoing antidepressant therapy to work closely with a healthcare provider to monitor their progress and make any necessary adjustments to their treatment plan to optimize their response and minimize side effects.
Antidepressant response is not solely reliant on medication; it often goes hand in hand with psychotherapy and lifestyle changes. Many individuals benefit from a combination of medication and therapy to address the underlying causes of their depression and learn coping strategies. The goal is not just symptom relief but also long-term emotional well-being and resilience.
How Antidepressant Response is measured
Antidepressant response is typically measured through a combination of clinical assessments and self-reporting by the individual undergoing treatment. Here are some common methods used to gauge antidepressant response:
1. Symptom Rating Scales: Healthcare providers often use standardized rating scales to assess the severity of an individual’s depressive symptoms before and during treatment. One widely used scale is the Hamilton Rating Scale for Depression (HAM-D) or the Montgomery-Åsberg Depression Rating Scale (MADRS). These scales consist of a series of questions or statements that assess the presence and severity of various depressive symptoms. The scores on these scales provide a quantitative measure of symptom improvement over time.
2. Self-Reporting and Questionnaires: Patients are frequently asked to complete self-report questionnaires, such as the Beck Depression Inventory (BDI) or the Patient Health Questionnaire-9 (PHQ-9), which assess their own feelings and experiences related to depression. These questionnaires provide valuable insight into the individual’s perspective on their mood and functioning.
3. Clinical Observation: Healthcare providers also rely on their clinical judgment and observations during therapy sessions or appointments. They assess changes in the individual’s demeanor, behavior, and overall well-being. This subjective assessment can complement the objective data gathered from rating scales and questionnaires.
4. Functional Improvement: Antidepressant response isn’t limited to symptom reduction; it also involves improvements in an individual’s daily functioning and quality of life. Healthcare providers may inquire about changes in the individual’s ability to perform everyday tasks, maintain relationships, and engage in activities they enjoy.
5. Side Effect Monitoring: It’s essential to monitor and manage any side effects that may arise from antidepressant medications. Any adverse effects that impact the individual’s overall well-being should be addressed and, if necessary, may lead to adjustments in the treatment plan.
Better Ways to Measure Antidepressant Response According to New Research
New research challenges the conventional approach to assessing patient response to antidepressant treatment by expanding the definition of “responder” and questioning the emphasis on symptom reduction alone. In a study involving over 800 patients with major depressive disorder (MDD), researchers found that while fewer than 40% of patients were classified as treatment responders based on symptom improvement, two-thirds met the criteria for responders when considering broader aspects of life satisfaction and improvement in functioning, as measured by the Patient Global Rating of Improvement (PGI) scale. This suggests that many patients may perceive significant benefits from treatment, even if their depressive symptoms haven’t met the traditional threshold of a 50% or greater improvement.
The study, conducted by Dr. Mark Zimmerman and published in the Annals of Clinical Psychiatry, underscores the importance of measuring outcomes beyond symptom severity in depression treatment. While symptom reduction remains a vital component of treatment, factors such as overall functioning, quality of life, and the ability to cope with life’s challenges are equally critical for patients’ well-being. Dr. Zimmerman suggests that multidimensional questionnaires that assess these broader aspects alongside symptoms may better align with patients’ treatment goals and provide a more comprehensive view of treatment efficacy. This research challenges the field to consider alternative methods for evaluating antidepressant responses that better capture the holistic well-being of individuals undergoing treatment for depression.
Overall, assessing antidepressant response is a multifaceted process that combines objective measures like rating scales with subjective information from the individual’s own experience. It’s important to track progress over time to determine the effectiveness of the treatment and make any necessary adjustments to optimize outcomes. Additionally, open communication between the individual and their healthcare provider is crucial to ensure that the chosen treatment approach is tailored to their specific needs and preferences.

