What Pill Is M 751?
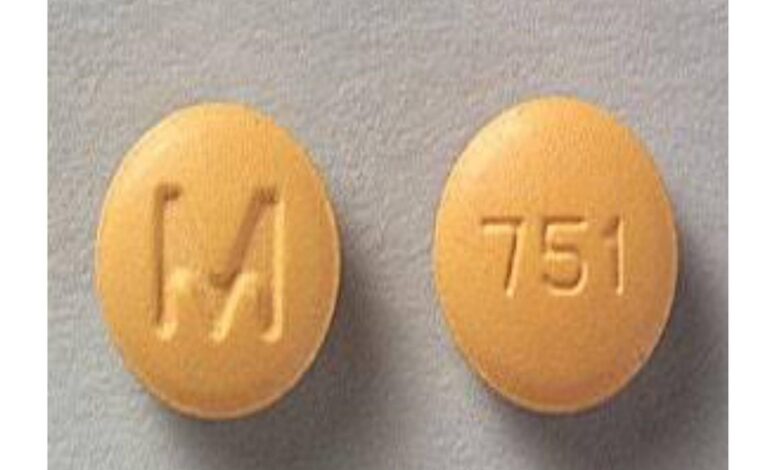
The yellow, round pill with the imprint M 751 has been identified as Cyclobenzaprine Hydrochloride 10 mg supplied by Mylan Pharmaceuticals Inc.. Cyclobenzaprine is used with rest, physical therapy, and other measures to relax muscles and relieve pain and discomfort caused by strains, sprains, and other muscle injuries. Cyclobenzaprine is in a class of medications called skeletal muscle relaxants. It works by acting in the brain and nervous system to allow the muscles to relax.
Cyclobenzaprine, is a centrally-acting muscle relaxant and was first synthesized in 1961. It has been available for human use since 1977. Cyclobenzaprine was approved for medical use in the United States in 1977. It is available as a generic medication. In 2018, it was the 43rd most commonly prescribed medication in the United States, with more than 18 million prescriptions. It was not available in the United Kingdom as of 2012.
How should the M 751 pill be used?
Do not take this drug for more than 3 weeks without talking to your doctor. Follow the directions on your prescription label carefully, and ask your doctor or pharmacist to explain any part you do not understand. Take cyclobenzaprine exactly as directed. Do not take more or less of it or take it more often than prescribed by your doctor.
What side effects can this medication cause?
M 751 pill may cause side effects. Tell your doctor if any of these symptoms are severe or do not go away:
- dry mouth
- dizziness
- nausea
- constipation
- heartburn
- extreme tiredness
If you experience any of the following symptoms, call your doctor immediately:
- skin rash
- hives
- swelling of the face or tongue
- difficulty breathing or swallowing
- irregular or fast heart rate
- chest pain
M 751 Pill Safety information
M 751 Pill contains cyclobenzaprine before taking this medication ;
- tell your doctor and pharmacist if you are allergic to cyclobenzaprine, any other medications, or any of the ingredients in cyclobenzaprine tablets or capsules. Ask your pharmacist for a list of the ingredients.
- tell your doctor if you are taking the following medications or have stopped taking them within the past two weeks: monoamine oxidase (MAO) inhibitors, including isocarboxazid (Marplan), phenelzine (Nardil), rasagiline (Azilect), selegiline (Eldepryl, Emsam, Zelapar), and tranylcypromine (Parnate). Your doctor will probably tell you not to take cyclobenzaprine if you are taking one of these medications.
- tell your doctor and pharmacist what other prescription and nonprescription drugs, vitamins, nutritional supplements and herbal products you are taking or plan to take. Be sure to mention any of the following: medications for allergies, coughs, or colds; barbiturates such as butabarbital (Butisol), phenobarbital, and secobarbital (Seconal); bupropion (Aplenzin, Forfivo XL, Wellbutrin, Zyban); meperidine (Demerol); sedatives; sleeping pills; selective serotonin reuptake inhibitors (SSRIs) such as citalopram (Celexa), escitalopram (Lexapro), fluoxetine (Prozac, Sarafem, Selfemra, in Symbyax), fluvoxamine (Luvox), paroxetine (Brisdelle, Paxil, Pexeva), and sertraline (Zoloft); selective serotonin and norepinephrine reuptake inhibitors (SNRIs) such as desvenlafaxine (Khedezla, Pristiq), duloxetine (Cymbalta), levomilnacipran (Fetzima), milnacipran (Savella) and venlafaxine (Effexor); tranquilizers; tricyclic antidepressants (TCAs) such as amitriptyline, amoxapine, clomipramine (Anafranil), desipramine (Norpramin), doxepin (Silenor), imipramine (Tofranil), nortriptyline (Pamelor), protriptyline (Vivactil), and trimipramine (Surmontil); tramadol (Conzip, Ultram, in Ultracet); verapamil (Calan, Covera HS, Verelan, in Tarka); or any other medication for depression, mood, anxiety, or thought disorder. Your doctor may need to change the doses of your medications or monitor you carefully for side effects. Many other medications may also interact with cyclobenzaprine, so be sure to tell your doctor about all the medications you are taking, even those that do not appear on this list. ;
- tell your doctor if you are recovering from a recent heart attack, or if you have an overactive thyroid gland, heart failure (condition in which the heart is unable to pump enough blood to the other parts of the body), or an irregular heartbeat, heart block, or other problems with the electrical impulses of your heart. Your doctor will probably tell you not to take cyclobenzaprine.
- tell your doctor if you have increased pressure in the eye or glaucoma, difficulty urinating, or liver disease.
- tell your doctor if you are pregnant, plan to become pregnant, or are breastfeeding. If you become pregnant while taking cyclobenzaprine, call your doctor immediately.
- talk to your doctor about the risks and benefits of taking cyclobenzaprine if you are 65 years of age or older. Older adults should not usually take cyclobenzaprine because it is not as safe or effective as other medications that can be used to treat the same condition.
- you should know that this drug may make you drowsy. Do not drive a car or operate machinery until you know how cyclobenzaprine affects you.
- ask your doctor about the safe use of alcoholic beverages while you are taking cyclobenzaprine. Cyclobenzaprine can make the effects of alcohol worse.